Blog
Article
Blog: Managing patients with MGD and Demodex blepharitis
Author(s):
(Image Credit: AdobeStock/Alessandro Grandini)
Because “dry eye” is often a multifactorial problem, solving it may require a multi-pronged approach. First, keep in mind that most of our dry eye patients, up to 86%, actually have evaporative dry eye.1 They produce plenty of tears, but the tear film is of poor quality. In meibomian gland dysfunction (MGD), the glands do not produce enough oil (meibum) or the oil is of poor quality, affecting the ability to spread over the ocular surface, increasing tear break-up time (TBUT), and provoking symptoms. Over time, this can result in inflammation, even though the original cause may not have been inflammatory.
Now that I’m looking for it closely, I increasingly find that many of my MGD patients also have Demodex blepharitis (DB). Historically, DB was diagnosed on the basis of microscopy-aided mite counts, which are impractical in clinical practice. There is now a consensus that DB can be diagnosed simply by the presence of collarettes, a pathognomonic sign, on the lashes.2,3
Collarettes are visible on the upper lashes of a patient with Demodex blepharitis. (Image courtesy Alice Epitropoulos, MD)
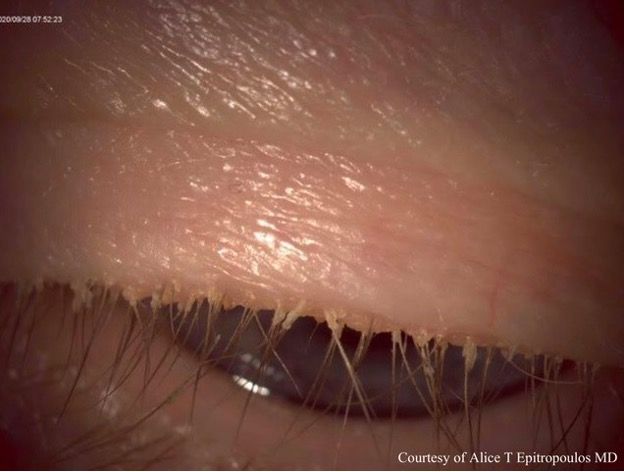
At the slit lamp, instruct the patient to look downward and focus on the lash margin of the upper lid. Collarettes, or sleeve-like debris at the base of the lashes, are a pathognomonic sign of Demodex mite overgrowth. Bacteria carried by the mites can in turn increase the risk of infection and potentially endophthalmitis, so it is particularly important to screen for DB in preoperative patients undergoing cataract surgery.
In cases like this, it really doesn’t matter which came first. Getting rid of the mites won’t necessarily unblock the meibomian glands, and getting the meibum flowing again may only partially resolve symptoms if DB persists. We have to treat all of it. Thanks to recent approvals, we now have a whole slate of synergistic treatments to help patients with concomitant MGD and DB.
I like to start with microblepharoexfoliation (BlephEx). I have for years combined this with thermal pulsation treatments because it effectively exfoliates the lid margin and gets rid of the accumulated biofilm that contributes to the inflammatory process. I expect it will also help prepare the lids for the newly approved therapy for DB, lotilaner ophthalmic solution, 0.25%. (Xdemvy, Tarsus Pharmaceuticals), which directly targets Demodex mites. Published data on the efficacy of Xdemvy is impressive. After 6 weeks of twice-daily drops, 56% of patients had grade 0 collarettes (0-2 lashes with collarettes) and 89% had grade 0 or 1 (≤10 lashes with collarettes). More than half the patients had total mite eradication and nearly one-third had no more erythema.4
After eradicating mites, I treat the patient with LipiFlow vectored thermal pulsation (Johnson & Johnson Vision). There are several other thermal pulsation systems, but LipiFlow has the longest history and the most peer-reviewed data behind it, demonstrating solid efficacy that lasts up to 3 years.5,6 Thermal pulsation is an extremely effective way to painlessly unclog obstructed or inspissated meibomian glands by warming the meibum (posterior and anterior eyelids) and then using consistent, pulsating pressure to gently express the glands.
Finally, I also like to prescribe Miebo (perfluorohexyloctane ophthalmic solution, Bausch + Lomb), a new nonaqueous therapy for evaporative dry eye. Miebo is comprised only of the active ingredient perfluorohexyloctane, so there are no excipients or preservatives to irritate the eyes. The drop inhibits evaporation by forming a monolayer at the air-tear interface to prevent evaporation, mimicking a key function of the natural meibum. It also promotes healing of the ocular surface. In the pivotal trials there were statistically and clinically significant improvements in eye dryness scores and total corneal staining.7,8 My expectation is that these drops will extend the benefits of LipiFlow.
All four of these treatments—blepharoexfoliation, lotilaner ophthalmic solution, thermal pulsation, and perfluorohexyloctane—can synergistically address our most common lid diseases, MGD and DB.
Following the in-office and prescription therapies, I like to put these patients on supportive maintenance therapies at home, as well.In my practice, this would include the re-esterified triglyceride (rTGC) form of omega-3 supplements. In the right dose, form, and ratio, omega-3 supplements have been shown to improve the composition of meibum and the signs and symptoms of dry eye.9,10 I also recommend a tea tree oil-based lid hygiene cleanser or wipes, and warm compresses. To some clinicians, this may sound like a lot to throw at the ocular surface, but I see it as analogous to the way that dentists treat and prevent plaque buildup around the teeth and gums: You get a deep cleaning at the dentist's office but then you also need to brush, floss, and use fluoride at home to maintain the benefits. For my patients with lid disease, a home regimen is going to support and extend the benefits of more targeted treatments, even though it can’t replace them.
References:
Lemp MA, Crews LA, Bron AJ, et al. Distribution of aqueous-deficient and evaporative dry eye in a clinic-based patient cohort: a retrospective study. Cornea 2012;31(5):472-8.
Ayres BD, Donnenfeld E, Farid M, et al. Clinical diagnosis and management of Demodex blepharitis: The Demodex Expert Panel on Treatment and Eyelid Health (DEPTH). Eye (Lond) 2023;37(15):3249-55.
Rhee MK, Yeu E, Barnett M, et al. Demodex blepharitis: A Comprehensive review of the disease, current management, and emerging therapies. Eye Contact Lens 2023;49(8):311-8.
Gaddie IB, Donnenfeld ED, Karpecki P, et al. Lotilaner ophthalmic solution 0.25% for Demodex blepharitis: Randomized, vehicle-controlled, multicenter, phase 3 trial (Saturn-2). Ophthalmology 2023;130(10:1015-23.
Lane SS, DuBiner HB, Epstein RJ, et al. A new system, the LipiFlow, for the treatment of meibomian gland dysfunction. Cornea 2012;31(4):396-404.
Greiner JV. Long-term (3 year) effects of a single thermal pulsation system treatment on meibomian gland function and dry eye symptoms. Eye Contact Lens 2016;42(2):99-107.
Tauber J, Berdy GJ, Wirta DL, et al. NOV03 for dry eye disease associated with meibomian gland dysfunction: results of the randomized phase 3 GOBI study. Ophthalmology 2023;130(5):516-24.
Sheppard JD, Kurata F, Epitropoulos AT, et al. NOV03 for signs and symptoms of dry eye disease associated with meibomian gland dysfunction: the randomized phase 3 MOJAVE study. Am J Ophthalmol2023;252:265-74.
Epitropoulos AT, Donnenfeld ED, Shah ZA, et al. Effect of oral re-esterified omega-3 nutritional supplementation on dry eyes. Cornea 2016;35(9):1185-96.
Smith SG, Gross MB, Sandnes OE, Physicians Recommended Nutriceuticals, LLC. Methods for improving the quality of the meibum composition of meibomian glands. U.S. Patent No. 9,381 183 B2, July 5, 2016.
Newsletter
Don’t miss out—get Ophthalmology Times updates on the latest clinical advancements and expert interviews, straight to your inbox.





