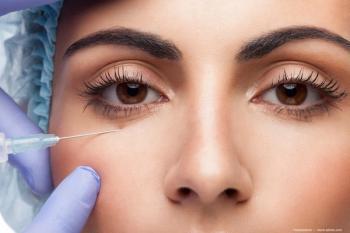
Treating chalazion with IPL therapy
IPL’s mechanism of action a useful tool in treating underlying causes of chalazia, according to Laura M. Periman, MD.
Editor’s Note: Welcome to “
Chalazion, that telltale “red bump” on the eyelid indicating an inflammatory lesion on a meibomain gland, is a fairly common sight in our practices.
Traditionally, we’ve sent patients home with warm compresses and a topical steroid/antibiotic drop or ointment. When these conservative measures fail, the lesions may require incision and drainage or an injection of triamcinolone acetonide (
IPL is indicated for benign inflammatory skin lesions. It is quite logical within that indication to treat inflammatory lesions on the skin of the eyelid with IPL technology and appropriate ocular protection in place.
There is a natural marriage between IPL’s mechanisms of action and the underlying causes of chalazia. IPL has demodicidal, anti-inflammatory, and anti-microbial, anti-telangiectatic properties, all of which address the inflammatory nature of chalazia. In addition, IPL features photobiomodulation, a process that stimulates cell mitochondria, promoting healthy cell function.
Using sixth-generation IPL technologies (
RELATED:
With IPL, we’ve also had success in resolving chronic chalazia (typically resolves in 2 weeks) that persisted despite previous incision and drainage procedures, home care, and medications.
Our patients really like that we offer a treatment option without drugs, drops, injection, or incision. They appreciate the reduced home care burden as well. (Warm compresses and BID are marginally effective and represent a significant compliance challenge for patients.)
We often see people who have an upcoming job interview or vacation, and they want help fast. For vacationers, clinicians want to avoid wound exposure during swimming and other activities. IPL is fast, effective, and incision-free, so there is no
One IPL treatment is usually enough for acute chalazia, and our patients tell us that acute chalazia are gone in 3 to 5 days. It’s hard to make the problem disappear that quickly with other modalities.
Patients appreciate several aspects to IPL for chalazia: the incision-free, injection-free, and medication-free approach; the speed, comfort, and completeness of IPL therapy; the effectiveness in addressing underlying comorbidities that contributed to the chalazion in the first place; and the potential to reduce the incidence of future chalazia.
My patients with a history of frequent chalazia report back that the frequency is greatly diminished.
RELATED:
Disclosures:
Laura M. Periman, MD
E: [email protected]
Laura M. Periman, MD, Ocular Surface Disease Expert and Director of Dry Eye Services and Clinical Research at Evergreen Eye Center in Seattle, WA. She discloses a relationship with Allergan, Bruder, BioTissue, Eyedetec, Lumenis, Science Based Health, Shire, Sun, TearLab and Visant.