Publication
Article
Digital Edition
Payment models for imaging: Procedures not covered by insurance policies
Author(s):
Tips to help eye care providers navigate the maze of insurance issues.
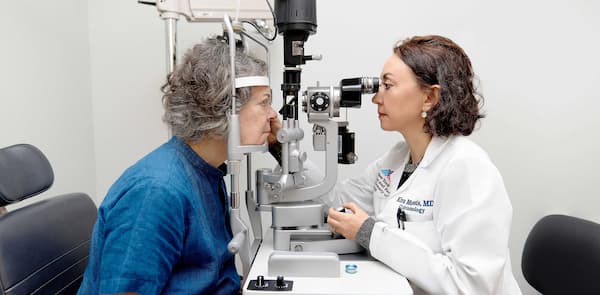
Eye care providers must navigate the medical and vision insurance payment landscapes while maintaining the highest quality of care. (Image Credit: Adobe Stock/dragonstock)

One reality of ophthalmic and optometric practice is that eye care providers must navigate the medical and vision insurance payment landscapes while maintaining the highest quality of care. In some cases, patients receive thorough examinations within the coverage parameters of their plans. In other cases, insurance coverage does not extend to imaging that providers may deem fundamental to a complete ocular evaluation.
How do eye care providers best manage this situation? Here, we offer a framework to consider when strategizing your practice’s approach to this challenge.
Different images for different scenarios
Most patients grasp the general concept that imaging allows an eye care provider to effectively evaluate their anatomy, and many clinicians insist on acquiring particular imaging reports in specific settings.
For example, optical coherence tomography (OCT) of the retina before cataract surgery is a necessary element of presurgical evaluation, and patients understand the value of that modality when their surgeon shows them their imaging results and explains how those results informed a surgical plan. Ultra-widefield (UWF) imaging, too, is useful in presurgical settings because knowledge of peripheral pathology that may otherwise go undetected may inform treatment approaches.
Retinoschisis, which was determined to be linked with a retinal detachment, was detected on ultra-widefield imaging during a 13-year-old patient’s first routine eye exam. (Image courtesy of Douglas Katsev, MD)
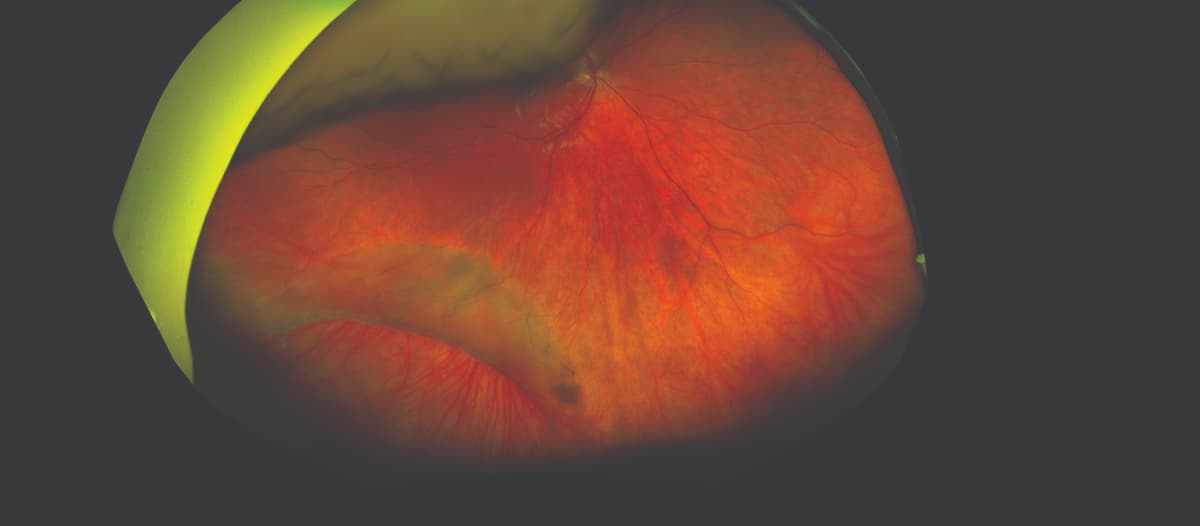
Thousands of published studies confirm the value of single-capture UWF imaging in eye care and for presurgical evaluation. A systemic literature review by Ahmed et al found that use of macular OCT screening resulted in detection of macular pathology in approximately 14% of presurgical cataract patients who were otherwise characterized as normal on funduscopic examination alone.1
Liu et al showed that with optomap UWF imaging, 92% of peripheral retina lesions were detected prior to refractive surgery.2 Our vitreoretinal colleagues have outlined the value of UWF imaging in multiple studies, showing that it both detects peripheral pathology that results in more nuanced disease diagnosis in diabetic eye disease3 and is capable of detecting pathology outside the 7 standard fields in more than 4 in 10 eyes of patients with retinal vascular pathology.4 Further, a 2021 survey of Optos device users documented that more than 97% of doctors using optomap imaging have found unanticipated pathology in an asymptomatic patient.5
UWF imaging is not exclusively a tool for retina practices. We have found that UWF photography is particularly useful in routine exam settings because it allows clinicians to quickly evaluate and document 200° of the retina.6 UWF imaging is also useful for documenting longitudinal data: When we have images of patients from multiple time points, we can better assess how their anatomy has changed over time. Although it takes an extra (but very brief) step to capture UWF images, many clinicians report that an UWF photo actually improves the efficiency of dilated fundus examination because the image can help focus the exam and point the provider to regions worthy of closer examination.
Billing and payment models
We should note that although ophthalmologists and optometrists use UWF imaging for similar reasons, important distinctions in their use are relevant to payment considerations. Ophthalmologists, particularly during presurgical evaluations or when managing retinal disease, document a medical necessity for the test, allowing direct billing of medical insurance. Optometrists, whose offices sometimes bill vision insurance rather than medical insurance, use UWF for screening purposes, and it often is not covered by patients’ vision plans. Still, the optometric utility of UWF, as we’ll discuss, is particularly high when one considers that establishing an imaging history is fundamental to providing high-quality, long-term primary eye care.
Because some insurance plans do not cover UWF imaging, practices must decide whether to forgo this helpful procedure, do the procedure without compensation, or ask the patients to bear some of the cost. There are various models for recovering imaging costs— some are easier than others to implement. Let’s review some of those methods.
Billable medical imaging
When performing UWF imaging in patients with established pathology who are enrolled in medical insurance, billing medical insurance for fundus photography is fairly straightforward. In this case, patients leave the clinic with no imaging-related out-of-pocket expenses.
Imaging cost incorporated into patient exam fee
In primary eye care settings, patients who present without insurance generally agree up front to pay for their exam. In these cases, cost of UWF imaging can be incorporated into the exam fee. In surgical scenarios, many surgeons insist that patients undergo OCT and UWF imaging before cataract surgery to minimize the risk of a preexisting retinal condition complicating surgical outcomes. Imaging is critical in this situation because it helps the doctor more effectively examine the retina through the patient’s cataract. In these cases as well, the costs of the imaging procedures are often incorporated into the overall cost of cataract surgery.
Patient pays out of pocket for uncovered imaging
When insurance does not cover UWF imaging, patients often elect
to pay directly for the procedure. Take, for example, a patient whose vision insurance covers the cost of a dilated exam but not the cost of a UWF fundus photo. In this case, the provider can explain the value of UWF imaging and ask the patient if they wish to add the cost as an out-of-pocket expense. I explain that UWF imaging is proven to increase the effectiveness of the exam and that keeping the images on file improves the ability to detect any changes over time. I also educate patients that image collection mitigates any hiccups when transferring between providers because their new clinician will be able to confidently and efficiently assess the patient’s history with objective imaging data.

If patients have further questions about the value of UWF imaging, discussing its utility in a real-world example of quiescent disease detection (such as that in the Sidebar) may be illustrative of UWF imaging’s value.
Providing top care and patient choice
Instances in which patients and providers discuss payment may make some clinicians uncomfortable. Rather than framing the discussion about out-of-pocket costs as one of nickel-and-diming patients, consider the discussion an opportunity to give patients agency in their own care and to educate them about the value of cutting-edge technology in your clinic. Doing so not only provides context for the value of continued examination but also empowers patients to take control of their ocular health.
Douglas Katsev, MD
E: katsev@aol.com
Katsev is the founder and surgical director of Santa Barbara Eyecare in California.
Julia Katsev Larson, OD
E: kkatsev@gmail.com
Larson is an associate optometrist and the marketing director at Santa Barbara Eyecare.
References:
Ahmed TM, Siddiqui MAR, Hussain B. Optical coherence tomography as a diagnostic intervention before cataract surgery-a review. Eye (Lond). Published online December 14, 2022. doi:10.1038/ s41433-022-02320-y
Liu L, Wang F, Xu D, Xie C, Zou J. The application of wide-field laser ophthalmoscopy in fundus examination before myopic refractive surgery. BMC Ophthal- mol. 2017;17(1):250. doi:10.1186/s12886-017-0647-4
Silva PS, Horton MB, Clary D, et al. Identification of diabetic retinopathy and ungradable image rate with ultrawide field imaging in a national teleophthalmology program. Ophthalmology. 2016;123(6):1360-1367. doi:10.1016/j.ophtha.2016.01.043
Jones NP, Sala-Puigdollers A, Stanga PE. Ultra-widefield fundus fluorescein angiography in the diagnosis and management of retinal vasculitis. Eye (Lond). 2017;31(11):1546-1549. doi:10.1038/ eye.2017.93
Dhoot D, Kitchens JW, Lahners W, Martinez C. Advances in Imaging Online Symposium, Pentavision, 2021.
Kumar V, Surve A, Kumawat D, et al. Ultra-wide field retinal imaging: a wider clinical perspective. Indian J Ophthalmol. 2021;69(4):824-835. doi:10.4103/ ijo.IJO_1403_20

Newsletter
Don’t miss out—get Ophthalmology Times updates on the latest clinical advancements and expert interviews, straight to your inbox.