News
Article
Digital Edition
New IOL is a go-to option for pseudoexfoliation syndrome, other challenges
Author(s):
Lens is stable in capsular bag, less sensitive to misalignment.
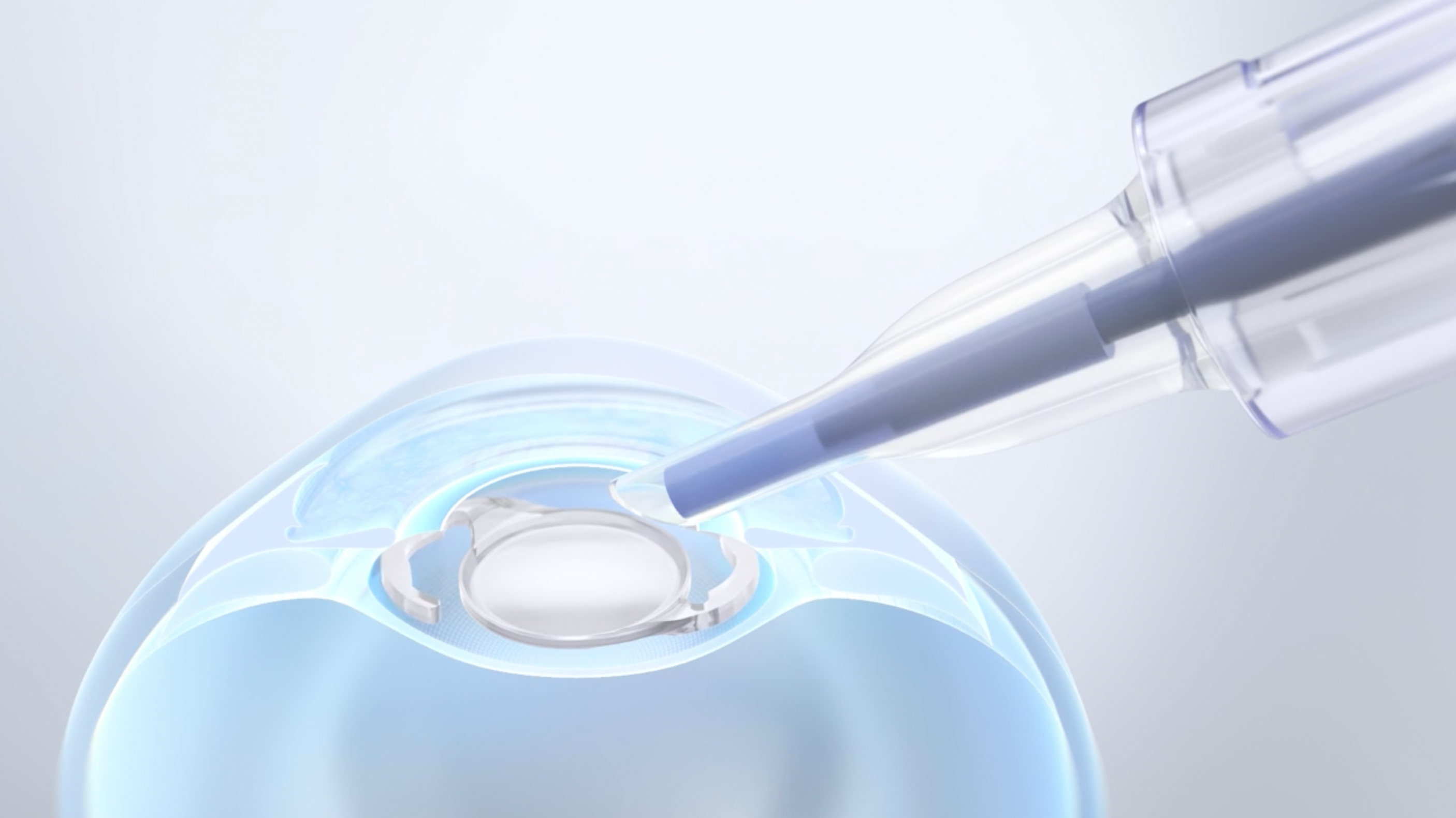
CT LUCIA 621P | Image credit: ©ZEISS
Reviewed by Andreas F. Borkenstein, MD
A new hydrophobic, acrylic, and aspheric 1-piece IOL (CT LUCIA 621P; ZEISS) may prove useful for patients with pseudoexfoliation syndrome (PXF) by providing greater stability in the capsular bag and less sensitivity to misalignment. Andreas F. Borkenstein, MD, reported the 2-year outcomes with this recently FDA-approved aspheric lens in a presentation at the American Society of Cataract and Refractive Surgery Annual Meeting 2023 in San Diego, California.
Careful lens selection is paramount in difficult cases or cases in which decentration is more likely, Borkenstein emphasized. Based on results from laboratory experiments in which he and coauthor Eva-Maria Borkenstein, MD, analyzed the optic haptic junction and evaluated capsular bag contact, monofocal IOLs with the same overall diameter can behave differently in the eye. Moreover, the authors performed optical bench tests to compare spherical and aspheric optic designs when misaligned.
In eyes with PXF, there is an increased risk of intraoperative and postoperative complications. “In these cases,” Andreas explained, “the selection of the IOL is crucial to achieve the best long-term results. Aspheric IOLs have some advantages when perfectly centered but are more sensitive to misalignment [because of] capsular phimosis, shrinkage, and loose zonules.”
The patented ZEISS Optics (ZO) optical concept has a special nonuniform power distribution to increase depth of focus. There is a central zone with negative spherical aberration correcting positive spherical aberration of the cornea for best imaging quality. There is also a second peripheral zone with positive spherical aberration that increases decentration tolerance. The ZO concept is intended to combine advantages from aspheric and neutral lenses.
A systemic problem
PXF is an age-related, multifactorial systemic disease that is characterized by extracellular material in the eye and other tissues. In the eye, deposits are seen on the lens epithelium, corneal endothelium, pupillary border, iridocorneal angle, trabeculum, ciliary process, and zonules. PXF is associated with increased IOP, glaucoma, cataracts, decreased pupillary dilation, zonular weakness, and a risk of complications.
Eyes of patients with PXF have a 10-fold increased risk of surgical complications, Andreas pointed out. The most serious intraoperative complications include a dropped nucleus, lens dislocation, and lens subluxation. The most severe postoperative complications are the need for subsequent procedures, dropped IOL, IOL subluxation, IOL decentration, and development of cystoid macular edema.
Evaluation of the CT Lucia 621P
The investigators conducted a retrospective, consecutive case series of patients with cataracts who had received a diagnosis of pronounced PXF and loose zonules and underwent implantation of the IOL in their clinic. The investigators then reported the 2-year outcomes. The study was to assess the long-term visual performance of the CT Lucia 621P IOL, measured as the postoperative visual acuity (VA) and refractive predictability in challenging cases of severe PXF.
The primary end point was best-corrected distance VA at 2 years, and secondary end points were refractive predictability, decentration and tilt, shrinkage of capsule, posterior capsule opacification, and presence of glistenings.
The first study included 11 patients, almost 75% of whom were men (mean patient age, 74.6 years). The investigators found that the IOL maintained a good position in the eye and was stable in the capsular bag even after 2 years. No case of luxation or subluxation developed.
The IOL showed good results with satisfactory VA even in cases where minor decentration or tilt developed when phimosis/shrinkage occurred or weak zonules led to phacodonesis. The uncorrected and best-corrected VAs were stable during the 2-year period. Posterior capsule opacification developed in 1 case, and yttrium aluminum garnet capsulotomy was performed. The mean postoperative uncorrected distance and best-corrected distance VAs were 0.07 and 0.02 logMAR, respectively.
Andreas emphasized that even in cases of capsular phimosis and shrinkage with decentration and/or tilt, no subjective or objective deterioration in overall quality of vision could be measured. The ZO concept of the lens, which combines the benefits of aspherical and neutral lenses, seems to be advantageous in these cases. The takeaways from the study were:
The lens performed well in challenging cases and showed good VA results in long-term follow-up.
No deterioration of the overall optical quality was observed in cases of decentration or tilt.
The special features of this IOL (ie, the ZO concept and the specially designed optic haptic junction) seem to address the risk factors in challenging cases.
These results agree with results from laboratory experiments and optical bench analysis. More clinical studies with higher number of cases are planned.
Andreas F. Borkenstein, MD
E: crustalith@gmx.at
Andreas F. Borkenstein, MD, and Eva-Maria Borkenstein, MD, are in private practice in Graz, Austria, and have no financial interest in this subject matter.

Newsletter
Don’t miss out—get Ophthalmology Times updates on the latest clinical advancements and expert interviews, straight to your inbox.