- Ophthalmology Times: February 1, 2021
- Volume 46
- Issue 2
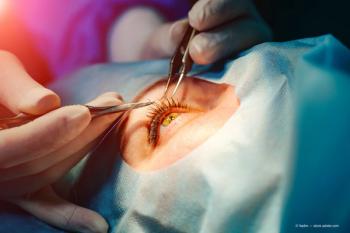
Iris-fixated IOLs are a boon for treating high myopia
Phakic lenses are proving to be excellent additions to refractive practices.
This article was reviewed by David R. Hardten, MD
When it comes to
According to David R. Hardten, MD, an adjunct professor of ophthalmology at the University of Minnesota in Minnetonka, surgeons offering LASIK or PRK by offering natural lens replacement and phakic IOLs can expand a practice’s range of refractive patients.
Hardten also noted that phakic IOLs are valuable in younger patients because accommodation is retained, and IOLs can treat high degrees of up to about 15 days. In addition, the accuracy achieved with this technology is excellent.
Related:
A downside is that complications can develop, such as angle closure, a crowded angle, decreased endothelial cell count, atonic iris, and cataract formation resulting from implantation of phakic IOLs that are too long or have enclavation that is too tight.
Therefore, careful preoperative evaluations are necessary to ensure that patients are good candidates for these IOLs.
Preoperative considerations
Preoperative planning is essential in cases in which a phakic IOL is being considered.
The anterior chamber depth (ACD) can be measured using the Pentacam (Oculus), ultrasound biomicroscopy (UBM), and optical coherence tomography to determine if there is adequate space in the anterior chamber (AC) to support a Verisyse (Johnson & Johnson Vision) or Visian ICL (STAAR Surgical). According to Hardten, 3.04 mm is considered a borderline ACD.
Hardten described a new technology, ClearScan (ESI, Inc.), which is a probe cover for any UBM instrument that provides distortion-free images, as well as improves the safety of the UBM, improves the safety and accuracy of imaging when measuring the ACD, and the sulcus-to-sulcus dimensions that are critical to implantation of the Visian phakic IOL.
Related:
The suggested safety parameters when implanting these IOLs is a 1.5 mm safety distance between the midperipheral iris at about 7 mm optical zone or between the top of an AC implant.
Surgeons should be aware that there is a growth of the lens with shallowing of the ACD of about 20 μm annually.
In patients with ACs that are too shallow to accommodate a phakic IOL, Hardten suggested that natural lens replacement might be a better option.
Hardten said he likes to use the Pentacam when planning implantation of both the Visian and Verisyse phakic IOLs because of the instrument’s software.
With the Visian IOL, the iris moves forward an average of about 0.44 mm after implantation, which is similar to the AC requirements to clear a Verisyse implant.
The Verisyse implant is not used often in the United States, but surgeons should be aware of the IOL’s enclavation.
Related:
“It is important to make peripheral iridotomies; the enclavation is done nasally and temporally. The paracenteses tend to be at the 10- and 2-o’clock positions oriented toward the midperipheral iris, where the enclavation will be done,” he said.
When implanting the Verisyse, knowing the patient’s ACD is important because of the possibility that the IOL centration can’t be finalized until the ACD is back to physiologic. He advised checking the centration with the physiologic ACD after enclavation.
Key insertion steps
The 6 mm Verisyse implant is best placed through a scleral incision due to the astigmatic effect. Hardten demonstrated the implantation procedure where he draws up a small amount of iris into the claw of the implant and then stabilizes the implant with forceps.
On the opposite side, a tuck of iris is created using an enclavation needle. The implant is rotated slightly posteriorly on the left side to draw the iris up into the claw, which helps hold the implant in place.
Related:
“These implants have been shown to be extremely safe over the long term if they are enclavated with enough iris but not so much that the implant is pushed back up against the iris and the natural lens, which can cause posterior synechiae,” he explained.
Postoperative procedures
Laser vision correction is possible after implantation of a phakic IOL. Hardten prefers to perform PRK for enhancements because of the large incisions that may have resulted in irregular astigmatism. The results are excellent. LASIK also could be performed if preferred by the surgeon.
Hardten reported a series of 22 eyes that were followed for a minimum of 1 month (mean, 5 months) after PRK and Verisyse IOL. The mean spherical equivalent at the last follow-up visit was +0.12, and the mean astigmatism was 0.25 d.
The uncorrected visual acuity (UCVA) was 20/25 or better in 82% and 20/40 or better in 95%. In eyes in which the original best-corrected visual acuity (BCVA) was 20/20, the UCVA was 20/25 or better in 94% and 20/30 or better in 100%. No eyes lost BCVA.
Related:
All patients implanted with phakic IOLs develop cataracts, requiring removal of the IOL and then cataract surgery. Hardten said he prefers to create a scleral incision to remove the Verisyse IOL and then creates a clear corneal incision for cataract removal and a new
He also prefers to use a capsular tension ring because of the potential for small areas of zonular dialysis in these cases because of the previous iridotomies and AC mobilization.
After the scleral incision is made in the explantation process, paracentesis is made like those created for enclavation. The incision is opened the full 6 mm length, adequate viscoelastic is injected, and a procedure opposite to that described for implantation is performed.
Following closure of the incision, standard cataract surgery can proceed temporally through the clear corneal incision.
Related:
Conclusion
Phakic IOLs are extremely useful in high myopia and an excellent addition to the refractive armamentarium of a practice. Enhancements are possible with PRK or LASIK.
These patients will eventually acquire cataracts that require removal, Hardten summarized.
---
David R. Hardten, MD
e:[email protected]
David R. Hardten, MD has a financial interest in Johnson & Johnson and ESI,. Inc.
Articles in this issue
over 5 years ago
Do you 'need' or just 'want' that new diagnostic imaging device?over 5 years ago
Noninvasive angiography with OCT offers definite valueover 5 years ago
Ophthalmology residents retrained as palliative care extendersover 5 years ago
How AAOOP is taking the pandemic by the hornsover 5 years ago
EyePod: Ophthalmologist shares Holocaust survival storyover 5 years ago
Investigators examine anti-VEGF medications in cases with ROP