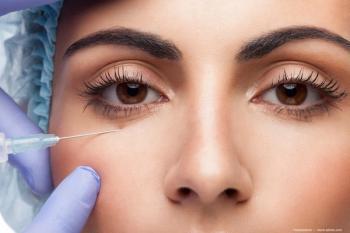
Could pandemic impact well-being of ophthalmologists?
A survey from The Larry A. Greene Center and the Primary Care Collaborative found that the COVID-19 pandemic is impacting the well-being of physicians.
Nearly half of primary care physicians reported that their burnout is at an all-time high, largely due to financial pressures caused by the COVID-19 pandemic, according to a new survey.
The survey, from The Larry A. Greene Center and the Primary Care Collaborative, found that the COVID-19 pandemic is impacting the well-being of physicians.
With physician burnout already a hot-button issue, the prospect of additional burden with the looming threat of COVID-19 could pose a real threat to clinicians, including ophthalmologists, moving forward.
Being a physician brings with it the ongoing struggle to balance work and personal life, and ophthalmologists are not immune to this issue. On the periphery is telemedicine, which could potentially lead to less burnout because physicians are able to optimize their schedules with efficient time management.
According to the Larry A. Green Center survey, of the physician respondents, 36% say their physical well-being has been suffered while 45% say their psychological well-being has suffered. A further 44% say that their personal burnout has reached an all-time high and 48 percent reported their office burnout is at an all-time high.
Compounding the issues, 63% of respondents are reporting that their stress is severe or near severe stress levels over the past week and 41% say they struggle to know when their workday ends.
According to the survey, the damage has moved beyond the physicians, with 65% of respondents saying the well-being of their families has suffered due to their work.
The survey found that the pandemic also continues to have a negative effect on practices, as 39% of respondents say that they have needed to layoff or furlough clinicians or staff. A further 25% of respondents say that they have skipped or deferred their own salaries, and another five percent reported that their practice is now temporarily or permanently closed, the survey says.
Some patients are still being seen as 60% of survey respondents report their non-face-to-face patient volume is at an all-time high. Meanwhile 60% of survey’s respondents noted they are limiting well and chronic care and 14% say they have had telehealth billing be denied.
When asked what they need to stay open, the top responses included:
- 21% need personal protective equipment as most have severely limited access to the equipment
- 16% need a return of in-person office visits as full workloads of non-in-person care is not enough to keep their practice viable
- 17% need financial assistance as increasing receivables are now inadequate for recovery from loss
- 12% need telehealth support to continue as it is becoming a key part of healthcare but not if the payment models is discontinued
Researchers in China conducted a separate cross-sectional study published in
The survey was fielded by The Larry A. Green Center, in partnership with the Primary Care Collaborative. The survey invitation was fielded June 12-15, 2020, with thousands of clinicians across the country.
In a separate Medscape survey, 22% of ophthalmologists reported feeling burned out, while just 3% reported feeling depressed. Only 8% reported feeling both.
Amid a potential increase in burnout during the pandemic, medical errors, physician suicide, and depression are serious consequences.
According to O’Brien, physicians should live in the moment, which can be achieved both by leaving their work in the office and not bringing it home to the family. This can start by putting down the phone or computer. Disconnect for a time from email, and patient charts. This can be even more important during the pandemic.
However, it is not all doom and gloom.
The Medscape survey also asked about those on the flip side — the happiest. Plastic surgeons were at the top (41%), followed by those in public health/preventive medicine (40%) and ophthalmologists (39%).
There also are ways to lighten the load.
While telemedicine can contribute to burnout with increased demands on working with technology, it also presents an opportunity to ease the burden on physicians. It can help with flexibility, including flexibility with the doctors and their schedule, and patients and their schedule because they able to reach the patients where they are at.
As a result, telemedicine can help ophthalmologists manage time, and it helps patients make sure that they can be seen in a timely fashion.
While burnout can be an issue for medical professionals, following expert advice for de-stressing, self-care, positive self-talk, and focusing on the present can help stave off burnout. Physicians also can reach out to their peers for psychological support.
Newsletter
Don’t miss out—get Ophthalmology Times updates on the latest clinical advancements and expert interviews, straight to your inbox.