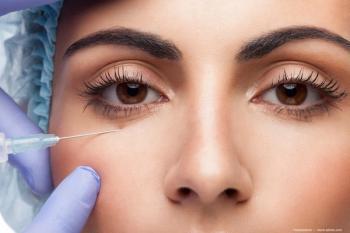
Blog: A call to stop discarding eye medications after a single use or before expiration date
In a blog, Mackenzie Andrews, the CCO and a co-founder of Nanodropper, discusses the need to update policies on single-use and early disposal of eyedrops.
Editor's note: The views expressed in this blog are those of their respective contributor and do not represent the views of Ophthalmology Times® or MJH Life Sciences®
Special to Ophthalmology Times®
Decades of habituation do not make regulatory policy and should be challenged. In a recent editorial in Ophthalmology titled, “Waste No More,” Wiley A. Chambers, MD, challenges existing institutional policies that require topical ophthalmic medications (eyedrops) to be discarded before the expiration date listed on the bottle.
We see Chambers as a fellow champion for reduced medical waste and increased access to medicine for taking a strong and common sense stance.
As a practicing ophthalmologist for more than 30 years, he argues, “Currently, some institutions have instituted policies and rules that require discarding ophthalmic drug products after a single use, despite the packaging being a multiple-dose container. These policies often lack a scientific basis and contribute to drug shortages that make it difficult for some physicians to obtain these products. I would like to suggest that it is past time to question these internal rules or policies.”
Chambers, while expressing his opinion in his capacity as a practicing ophthalmologist, currently serves as the director at the FDA’s Center for Drug Evaluation and Research in the Division of Ophthalmology.
“Artificial expiration dates, such as 28 days after opening on ophthalmic drug bottles, or restricting the use of ophthalmic drug bottles to a single patient use are not set with the same rigor,” Chambers stated after exploring the need for evidence-based decision making. “To the best of my knowledge, no scientific data support these artificial expiration dates or restrictions in use for topical ophthalmic drug products.”
Furthermore, there’s no regulatory requirement for early bottle disposal and Chambers’ research shows these policies are often based on misinterpreted rules from other organizations such as the FDA, USP, and TJC.
“As it turns out, none of these groups require a medication to be discarded before the expiration date listed on the bottle,” he said.
The pace of change in our healthcare system is admittedly glacial. However, it should not take another full lifetime to eliminate medical waste, increase access to medications, and decrease costs. A recent analysis finds that if multidose dropper bottles are safely used for multiple patients as intended, the cost savings amount to $284 per patient and $331 to the medical facility for every inpatient cataract case.
Policies around early bottle disposal are contributing to waste, drug shortages, rising healthcare costs, and are obstructing patient access to care. As advocates for data-driven decision making, and with Chambers among those advocating for change, we are pushing harder than ever for outdated policies on single-use and early disposal of eyedrops to change.