Study: Intravitreal bevacizumab in diabetic patients limits macular edema after cataract surgery
Speaking at AAO 2019, Ashraf El Habbak MD, PhD pointed out that bevacizumab inhibits vascular endothelial growth factor, which is a potent permeability factor implicated in cystoid macular edema.
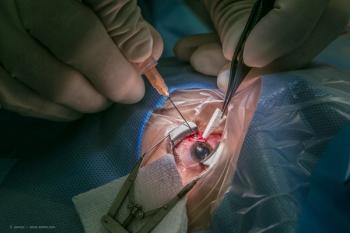
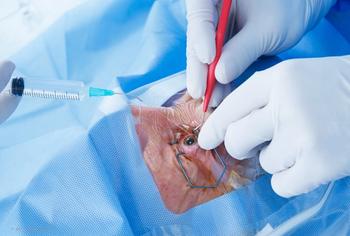
Intravitreal injection of bevacizumab (Avastin, Genentech) at the time of phacoemulsification in diabetic patients without maculopathy protected against the development of postoperative macular edema, according to the findings of a prospective, randomized comparative study reported by Ashraf El Habbak MD, PhD.
“There is an increased risk of cataract in patients with diabetes, and in fact, 20% of all patients who undergo cataract surgery have diabetes,” said Dr. El Habbak, professor of ophthalmology, Benha University, Banha, Egypt. “Macular edema after cataract surgery can adversely affect visual outcome, and Kim et al. reported that 22% of diabetic patients had a >30% increase in central retinal thickness after uncomplicated phacoemulsification.”
Dr. El Habbak also pointed out that intraocular surgery increases retinal vascular permeability, resulting in increased macular edema.
“Bevacizumab inhibits vascular endothelial growth factor, which is a potent permeability factor implicated in cystoid macular edema,” he said.
Using injections
Dr. El Habbak said that for the past 10 years, he has been injecting intravitreal bevacizumab at the end of cataract surgery in patients who have a ≥10-year history of diabetes and no maculopathy after such a patient developed severe macular pathology.
To formally assess the effect of this intervention, he conducted a prospective study that included 100 eyes of 65 patients. Eligible patients had a ≥10-year history of diabetes and no evidence of diabetic maculopathy.
Patients were excluded if they had a history of any ocular surgery, experienced intraoperative complications, had age-related macular degeneration or any other macular pathology, or if they had a recent history of myocardial infarction or cerebrovascular accident. The eyes were randomly selected to undergo phacoemulsification alone or combined with intravitreal injection of bevacizumab 1.25 mg delivered at the end of the case using a 30 G needle.
All surgeries were done under local anesthesia through a 2.4 mm clear corneal incision. All patients received the same single-piece, foldable, hydrophilic acrylic IOL in the capsular bag and the same anti-inflammatory medication regimen that included a topical corticosteroid and a topical nonsteroidal anti-inflammatory drug.
Central macular thickness
Central macular thickness (CMT) was measured before surgery and three months postoperatively using optical coherence tomography.
The results showed a statistically significant increase in CMT in the control group and a decrease in the eyes receiving intravitreal bevacizumab, although the change in the treated eyes was not statistically significant. In the control group, mean CMT increased by approximately 20% from 167.58 microns to 208.56 microns (P<.005).
In the eyes treated with intravitreal bevacizumab, mean CMT decreased by 3.5% from 65.86 μm at baseline to 160.12 μm at three months. Dr. El Habbak noted that the change in CMT measured in the control group is consistent with that reported in other studies of patients with diabetes.
ESCRS PREMED study
The multicenter randomly selected ESCRS PREMED study compared the addition of subconjunctival triamcinolone acetonide 40 mg, intravitreal bevacizumab 1.25 mg, a combination of both, or no additional treatment in 213 diabetic patients receiving topical corticosteroid and NSAID medications after uneventful cataract surgery.
The study found that intravitreal bevacizumab did not have a significant effect on macular thickness measured at six or 12 weeks after surgery compared with the controls. In the study, central subfield mean macular thickness was 12.3 μm and 9.7 μm lower, respectively, in patients who received triamcinolone acetonide than in patients who did not, and the difference between groups was statistically significant.
Postoperative IOP was also significantly higher in patients who received triamcinolone than in patients who did not, and the authors of the ESCRS PREMED study stated that the risk for developing cystoid macular surgery after cataract surgery in diabetic patients should be carefully weighed against the risk for treatment-related complications, such as increased IOP.
Disclosures:
Ashraf El Habbak MD, PhD
Dr. El Habbak has no relevant financial interest