- Ophthalmology Times: July 1, 2020
- Volume 45
- Issue 11
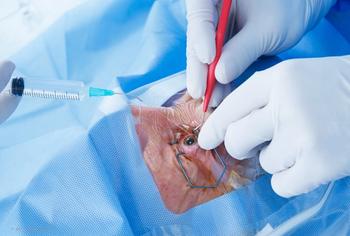
For IOL placement, location is key
Alternative method ensures lens is set properly during cataract surgery
Special to Ophthalmology Times©
The value of lens alignment technology for toric
However, a topic that is not as prevalent is how surgeons ensure that a multifocal IOL is centered on the visual axis during
Related:
Herein, I will share how I utilize lens alignment technology, not only for toric markings but also to verify the visual axis for multifocal lens implantation.
This approach has become critical for me to confirm proper placement and help decrease postoperative adverse events.
Finding the center of the visual axis
As cataract surgeons, we try to do our best at controlling variables so that we have more predictability with our outcomes.
As such, there are many preoperative tools at our disposal, including topography, aberrometry, ray tracing, or various alignment systems.
However, intraoperatively, only recently have we discovered an efficient way of applying the preoperative data we have collected and using them in the operating room.
Related:
Aberrometry has also been used intraoperatively, but its benefit is in the lens power and alignment of a toric
My colleagues and I have a variety of technologies that provide
Although we have an incredible amount of preoperative data, in surgery, we often find ourselves still guessing or “eyeballing” the placement of the lens.
For instance, in the past, we have used the Purkinje reflex of the microscope to align and center the lens, which can be affected by patient gaze. We often centered the lens based on the pupil.
However, if the pupil is irregular, we may not be placing it in the center of the visual axis, and some patients have a high-angle kappa or chord Mu (average chord mu, 0.2 ± 0.11 mm) where the center of the visual axis is not at the center of the pupil.
Related:
As a result, patients can have up to 0.5 mm to 0.6 mm of difference between the center of the pupil and the center of the visual axis.
Furthermore, if a patient has irregular or dilated pupils, it interferes with the ability to judge the location of the center of the visual axis due to the distorted pupil and iris.
An alternate approach
What I have found revolutionary about using a biometer with lens alignment technology (IOLMaster 700; Carl Zeiss) and a digital marking system (Callisto eye; Carl Zeiss) is that it allows me to use preoperative data and apply them intraoperatively to help position the lens in an efficient and consistent way.
Lens alignment technology gives me a true understanding of where the visual axis is located using swept-source optical coherence tomography with a cross-sectional B-scan view of the eye, allowing me to visually confirm the foveal pit.
Related:
Now I have an accurate and confirmatory measurement to ensure that my preoperative data actually measure the center of visual axis.
Of equal importance, the lens alignment technology takes images of the episcleral vessels preoperatively and can be applied to a digital marking system intraoperatively.
I am able to send the information to the digital marking system using digital software or I can transfer the data using a USB drive.
Intraoperatively, the digital marking software will register and align the scope view of vessels with the image taken by the lens alignment technology to ensure proper alignment.
For toric lenses this is ideal, because it allows me to apply my preferred axis of astigmatism.
For a multifocal lens, it will give me an overlay to create my capsulotomy of desired size. For instance, a 5-mm capsulotomy will center over the visual axis.
Also, once referenced, as the eye or scope moves so do the digital alignment markings. This can be invaluable as patients often have a hard time maintaining gaze, making it difficult to align capsulotomy and Purkinje reflexes.
Finally, at the end of the case, when I am putting the multifocal lens in the eye, there is a plus sign in the overlay that will tell me where the center of the visual axis is located, and it amazes me that this is not always exactly the center of the pupil.1
We have found that in patients with higher chord mu values, the digital visual axis alignment is often not aligned with the center of the pupil.
There is no doubt that multifocal lenses have an inherent higher risk of causing dysphotopsia due to the multifocal nature of the design in the lens.2,3
Related:
Glares, halos, and other dysphotopsias can be exacerbated if the patient is not looking through the center optic, especially the distant dominant optic. If the lens is not quite in the center of the visual axis and is positional slightly temporal to the visual axis, the patient might be looking through an edge of one of the rings, thus causing more postoperative symptoms.
To minimize this adverse event, I want the center of the multifocal
Conclusion
By using up-to-date formulas and advanced diagnostic tools, we can achieve a high probability of achieving our refractive target. Though we feel confident in achieving our targets, I can never guarantee a specific result to a patient. I always share with patients that there are risks and benefits to any procedure.
There is always a need, potentially, for enhancement or the possibility for something to go wrong. But when I have confidence in the technology, it is conveyed naturally.
I am not selling something; I am simply educating. And when I educate with confidence, it is easier for patients to consider the options.
About the author
Inder Paul Singh, MD
e:[email protected]
Paul Singh, MD, has no financial disclosures related to this content.
-----
REFERENCES
1. Zeng M, Liu Y, Liu X, et al. Aberration and contrast sensitivity comparison of aspherical and monofocal and multifocal intraocular lens eyes. Clin Exp Ophthalmol. 2007;35(4):355-360. doi:10.1111/j.1442-9071.2007.01452.x
2. Karhanová M, Pluháček F, Mlčák P, Vláčil O, Šín M, Marešová K. The importance of angle kappa evaluation for implantation of diffractive multifocal intra-ocular lenses using pseudophakic eye model. Acta Ophthalmol. 2015;93(2):e123-e128. doi:10.1111/aos.12521.
3. Tchah H, Nam K, Yoo A. Predictive factors for photic phenomena after refractive, rotationally asymmetric, multifocal intraocular lens implantation. Int J Ophthalmol. 2017; 10(2):241-245. doi:10.18240/ijo.2017.02.10
Articles in this issue
almost 6 years ago
Pearls for managing COVID-19 pandemic north of the borderalmost 6 years ago
Stepping up to meet visual needs of refugees in Bangladeshalmost 6 years ago
Investigators target algorithm for diagnosing glaucomaalmost 6 years ago
A sight for sore eyesalmost 6 years ago
The value of a reputation: Mixing medicine, politics a bitter pillalmost 6 years ago
Optimizing practice environment, outcomes, and patient satisfactionalmost 6 years ago
Ultra-widefield imaging can enhance efficiency for practicesalmost 6 years ago
Study targets results of MIGS device versus trabeculectomyalmost 6 years ago
Getting it right: There is no magic bullet for IOL calculationsalmost 6 years ago
Surgeons discuss MIPS, impact of pass-through medications