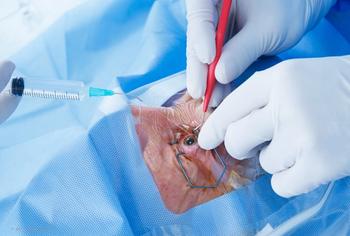
Setting expectations for glaucoma patients having cataract surgery
Pearls can ensure physicians get best outcomes, help patients set realistic goals
With planning and strategic use of surgical tips and techniques, physicians can lower the chance for vision loss in advanced glaucoma patients having cataract surgery.
Reviewed by Anup Khatana, MD
Setting expectations patients and physicians before cataract surgery in advanced glaucoma cases was one of eight pearls shared by
Dr. Ou focused her pearls on advanced glaucoma patients having cataract surgery. “All of us know many of these tips, but taken together, they can help minimize vision loss,” she said.
Here are Dr. Ou’s eight pearls:
1. Use careful surgical planning
Part of this planning process is deciding whether to do a staged procedure with glaucoma surgery performed first or do a combined procedure.
“Cataract surgery after a filtering procedure may pose a risk to the bleb, but combined surgery also may make some parts of surgery easier,” Dr. Ou said. One option is performing cataract surgery alone, while another pre-surgical plan involves IOL selection.
“Most of us will choose a monofocal IOL, but it’s also worthwhile to consider a toric,” she said.
There is research that shows greater astigmatic correction and good visual outcomes with the use of toric IOLs in this patient group but be careful with this choice in patients who have pseudoexfoliation, Dr. Ou cautioned. Dr. Ou also noted that physicians should avoid multifocal IOLs in advanced glaucoma patients.
2. Manage expectations
Physicians also should consider consenting for cataract surgery with or without bleb revision. “Patients with well-controlled or low IOP are less likely to have an IOP drop,” Dr. Ou said.
3. Take steps prophylactically to avoid an IOP spike
Patients with a longer axial length, prior laser trabeculoplasty, or who used a larger number of medications were more likely to have a spike in previous research, Dr. Ou reported. Oral acetazolamide, Miostat, and a topical beta blocker or a combination drop of beta blocker and carbonic anhydrase inhibitor all are options to help protect against IOP spikes.
4. Minimize inflammation
“Use all the methods at your disposal for a nice, dilated pupil,” Dr. Ou advised. Efforts to minimize inflammation could include visco dilation with Healon5 or several other iris expansion techniques. Thorough cortex removal also is important.
5. Remove viscoelastic material
Viscoelastic is necessary to maintain the anterior chamber depth throughout the procedure, especially in hyperopic eyes and those with prior filtering surgery. Complete removal can be a challenge, but take the extra time to do it, especially in high myopes, Dr. Ou said. Make sure to also remove viscoelastic material behind the IOL. A technique from
Avoid manipulation of the bleb and consider adding a 5-fluorouracil injection at the end of the case and during postoperative visits. To get a sense of bleb function intraoperatively, trypan blue can be used but is not always predictive, Dr. Ou said.
7. Maintain close follow-up
Spikes in IOP can occur four to six hours after surgery, so consider same-day postoperative visits for at-risk patients or a close follow-up to monitor for IOP spikes.
8. Consider use of steroids
The use of ophthalmic steroids is especially key if the surgeon sees early indications of bleb failure, Dr. Ou explained. Ophthalmic steroids, usually eye drops, gels, or ointments, are made to be administered in or around the eye. They also treat inflammation and relieve symptoms that can include pain, swelling, irrigation and redness.
Disclosures:
Yvonne Ou, MD
E: [email protected]
This article was adapted from Dr. Ou’s presentation at the American Glaucoma Society annual meeting. Dr. Ou is a consultant for Merck.