Image may be everything with ultrawidefield-guided swept-source OCT
Technology is an option for evaluating, documenting certain types of retinal pathology.
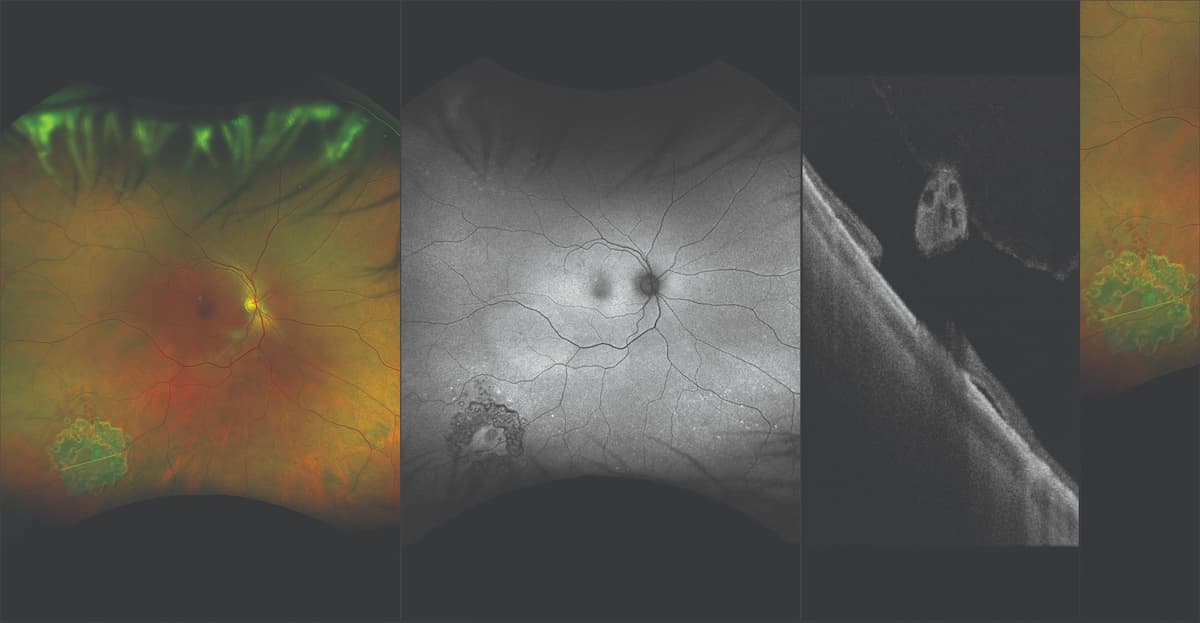
Ultrawidefield (UWF) RG scanning laser ophthalmoscopy (SLO) image, UWF autofluorescence SLO image, and optical coherence tomography image of treated operculated retina hole. (Image courtesy of David Brown, MD, Retina Consultants of Texas)
When it comes to adopting new therapies and technologies, physicians know to balance the excitement of possibilities with a healthy dose of pragmatism. Factors such as return on investment; practice efficiency; and, most importantly, patient benefit must be weighed in concert. Diagnostic tools and platforms are no exception.
The quality and quantity of information they deliver must add value yet also be captured and made accessible without sacrificing too much time or patient comfort and convenience. The following is an overview of factors to be considered in the case of ultrawidefield (UWF)-guided swept-source optical coherence tomography (SS-OCT) (Silverstone, Optos plc).
About Silverstone
Silverstone appears to be like the other Optos UWF imaging platforms, and indeed it offers the quality and array of imaging modalities that we have come to expect: UWF color, autofluorescence, fluorescein angiography (FA), and indocyanine green angiography optomap imaging. However, Silverstone is the only UWF imaging device that also features integrated UWF-guided SS-OCT scanning at any position in the 200° field of view.
UWF imaging and OCT have both earned their designations as invaluable diagnostic tools. Having the 2 modalities combined in 1 platform allows clinicians to identify and select any area of concern within the 200° field and produce an OCT image of that area for further evaluation (and documentation).
Clinical utility
While older patients are more likely to have pathology in the macula, younger patients, such as those seen in comprehensive ophthalmology and optometry, may have peripheral lesions without macular pathology or changes in vision, making this technology a valuable diagnostic tool for these practitioners. UWF-guided OCT might not be necessary for every patient; however, it can prove particularly useful in such cases.
For a peripheral pigmented lesion, a UWF-guided OCT can help ensure that there are no concerning features and therefore indicate that the lesion is benign.
In the case of peripheral retinal elevation where it is unclear whether or not it is retinoschisis, the platform provides the ability to image right at the edge of the schisis to determine whether it is an intraretinal separation of layers or subretinal fluid.
Moreover, documenting that it’s not a retinal detachment requiring urgent intervention is extremely reassuring to the clinician, the patient, and the referring doctor.2
Atrophic retinal holes can sometimes develop altered pigmentation around them, which can make it difficult to ascertain whether or not it’s the beginning of subretinal fluid pooling. In such instances, a UWF-guided OCT can help make that important distinction and avoid unnecessary laser treatment.
The evaluation
When a practitioner is evaluating a suspicious choroidal nevus, part of the criteria for assessing the progression or risk of a small melanoma is the presence of fluid overlying a lesion. It is obviously difficult to image peripheral nevi with traditional OCT. To be able to capture a UWF-guided OCT and document that the patient lacks that risk factor for choroidal melanoma will be very helpful.
Importantly, beyond this technology’s diagnostic value, it also enhances the ability to document extramacular lesions, including retinal tears, retinoschisis, suspicious nevi, and the leading edge of an exudative peripheral lesion such as a vasoproliferative tumor or peripheral exudative hemorrhagic chorioretinopathy.
Recent research
Some of these examples have been validated in the literature. A study published in the British Journal of Ophthalmology reported that UWF-guided SS-OCT helped detect retinal detachment, schisis-detachment, and retinoschisis in cases where the diagnosis was not clinically evident.1 In the same study, the authors reported that UWF-guided OCT uncovered vitreous adhesion at the posterior border of a retinal dialysis. These examples further underscore the technology’s potential as a tool for evaluating microstructural peripheral vitreoretinal pathology in real time, which thus far is a relatively unmet need despite the prevalence and clinical significance of this type of pathology.
UFW-guided OCT
The results of another publication indicated UWF-guided OCT may help distinguish intraretinal microvascular abnormalities from neovascularization elsewhere (NVE) and even reveal NVE that might otherwise go undetected by UWF alone.2 The gold standard for identifying proliferative diabetic retinopathy is UWF FA. However, the treatment burden is high given the invasive nature of this test, therefore making the potential for an alternative option such as UWF-guided OCT compelling.
Benefits beyond the clinic
In addition to the clinical benefits, UWF SS-OCT has tremendous potential as a research tool. UWF-guided OCT imaging has the potential to shed new light on peripheral pathology such as congenital hypertrophy of the retinal pigmented epithelium lesions, retinal cysts, or abnormalities at the ora serrata.
Conclusion
UWF-guided SS-OCT offers an efficient and effective option for evaluating and documenting certain types of retinal pathology in patients diagnosed with these diseases. The examples shared here demonstrate that there are a good number of cases many physicians encounter on a regular basis for which this technology would prove its utility. Moreover, the technology may also prove to be quite valuable as a research tool that leads to better understanding of a variety of peripheral pathologies.
Nikolas London, MD, FACS
P: 858-451-1911
London is president, director of research, and managing partner at Retina Consultants San Diego. He has no financial disclosures related to this content.
References:
1. Lee WW, Muni RH. Single-capture ultra-widefield guided swept-source optical coherence tomography in the management of rhegmatogenous retinal detachment and associated peripheral vitreoretinal pathology. Br J Ophthalmol. 2023;107(9):1356-1362. doi:10.1136/bjophthalmol-2021-320149
2. Ashraf M, Sun JK, Silva PS, Aiello LP. Using ultrawide field-directed optical coherence tomography for differentiating nonproliferative and proliferative diabetic retinopathy. Transl Vis Sci Technol. 2023;12(2):7. doi:10.1167/tvst.12.2.7
