How to boost your efficiency in the OR
Even small changes can have a large impact, saving time for physicians.
Image by Jennifer Toomey / MJH Life Sciences using AI

Surgical efficiency is an important metric that encompasses a variety of factors, including achieving safe and effective surgery with the least amount of effort, shaving valuable time from a surgery schedule, optimizing processes, and putting available resources to their best use. The first step in boosting your efficiency in the operating room (OR) is to determine exactly what you’re hoping to achieve.
I have spent the past few years focusing on performing better, faster, and more accurate surgery. Modern cataract surgery is extremely safe and efficient, and technological advances have led to more predictable surgery in fewer steps. It therefore can be challenging to find further efficiencies. Focusing on small changes while maintaining a routine is key.
Maintain routine
I like to perform my cataract surgery procedures with the same steps each time, but I will deviate from my routine for case-specific requirements such as in eyes with small pupils and posterior polar lenses. Performing the same steps of surgery in most cases helps me focus on achieving precise and effective movements, reducing surgical time and ensuring a safe procedure. Additionally, I like to use as few surgical steps as possible and only enter or exit the eye between steps to decrease surgical time and reduce the risk of tissue damage.
I also believe that simplifying steps, maintaining a routine procedure, and communicating effectively in the OR helps our staff perform better and leads to better staff buy-in. I am therefore able to train, delegate, and supervise our technicians to perform nonsurgical steps. These can include preparing the eye for surgery, draping the patient, and placing the eyelid speculum. This boosts our efficiency and the safety of the procedure.
In my OR, a routine cataract surgery procedure can be performed in about 10 minutes. Achieving a perfect workflow is crucial to staying on time and maintaining safety. Minimizing distractions and being ready to pivot to a new strategy when needed are also parts of the equation.
A complication interrupts routine but having the ability to react quickly can help maintain efficiency and get you back into the routine groove. For example, having a pupil-expanding device such as the I-Ring (BVI Medical) at the ready for potential intraoperative miosis can mean the difference between a few extra minutes added to the procedure time and managing a devastating complication.
Focus on small changes
IOL insertion. A great example of a small change that can make a big impact on efficiency is insertion of an IOL. At many academic centers and multispecialty ambulatory surgery centers, technicians are not always trained on how to load an IOL into an injector. A simple product such as preloaded IOLs saves surgeons in these settings time and helps boost the efficiency metric. It also cuts down on the number of scratched lenses, which when they occur can take away from surgical efficiency if a new IOL needs to be loaded.
I prefer the iPure family of preloaded hydrophobic IOLs (BVI), which fit through a 2.4-mm incision. As a complex anterior segment surgeon, it is comforting to know that I don’t need to look away from the surgical field to load the IOL. Additionally, I can avoid destabilizing the eye because the wound does not have to be enlarged like it might with other 3-piece IOLs.
I also find that selecting a handful of reliable IOL models, especially when they are preloaded, is helpful for technicians because they are less likely to fumble or make mistakes during surgery compared to with the use of a new or unfamiliar IOL. This can carve seconds off each case, which over the course of a 20- to 30-case day adds up to significant time savings.
Wound construction.Another small but important factor that can boost efficiency is wound construction. I typically create a 2.4-mm incision, and achieving a clean and triplanar entry is especially paramount in these cases to maintain a stable IOP and ensure the wound will self-seal.
The use of a sharp blade such as Beaver Knives (BVI) is crucial to saving time by avoiding the need to hydrate the wound multiple times at the end of a case. I have found that excellent wound construction also reduces the risk for hypotony on postoperative day 1. I like that the Beaver Knives have a depth indicator, which leads to a gentler insertion compared with other knives I have experience with.
Phacoemulsification. Keeping up to date with the latest phaco machines is also important. Newer-generation phaco systems have advanced fluid dynamics. Integrating a new technology can be costly, but it in turn helps with efficiency metrics. It can lead to a faster surgical technique and even allow more cases to be performed on surgery days.
Patient flow. One often overlooked and simple-fix efficiency boost is to consider your patient flow. How do patients move through your practice, from the time they check in to their preoperative preparations, surgical experience, and postoperative care? Enhancing patient flow can not only avoid bottlenecks but reduce the stress patients feel on the day of surgery. Similar questions should be asked about the OR layout. Is the scrub sink in a convenient location? Is the clean room as close as possible to the OR to avoid contamination in the unsterile hallway? Even little details matter when you are trying to boost efficiency.
Visualization in complex cases
Cataract surgery in complex cases is the one time when I try not to focus on efficiency. Maintaining efficiency in these situations is a double-edged sword. Truthfully, in any ocular surgery, getting in and out of the eye as quickly as possible is key to facilitate rapid postoperative wound healing and prevent corneal edema. The goal, however, is to perform routine, efficient surgery without rushing and taking undue risks.
I like to schedule all my difficult cases at the end of the day so that I don’t have to worry too much about time and can concentrate on safety. One area that I have found to be exceptionally important in this setting is visualization of the surgical field. When you start to lose the ability to visualize what you are doing, the risk of complications increases significantly. I prefer to perform heads-up 3D surgery with a digital surgical scope, which allows a higher level of magnification and resolution than a traditional microscope.
The magnification of 3D surgical systems is surreal, allowing me to visualize the surgical field down to the individual fibers on the posterior capsule. Seeing such detail provides me with peace of mind knowing that the posterior capsule remains intact during surgery or alerting me to any possible complexities I should avoid. Additionally, a surgeon filter can enhance tissue and membrane contrast.
Building efficiency with 3D heads-up surgery and integrating it into our daily system takes time. I was a little hesitant when I first started adopting the technology. As with anything, there was a learning curve, but it was not as lengthy as one would think. It took me about
2 or 3 cases to get comfortable with the Beyeonics One (BVI) platform. The ophthalmic exoscope, controlled through an immersive augmented reality surgical headset, is an intuitive imaging platform (Figure).
Figure: Eric D. Rosenberg, DO, MScEng, performs 3D heads-up surgery with the Beyeonics One ophthalmic exoscope. (Image courtesy of Eric D. Rosenberg, DO, MScEng)
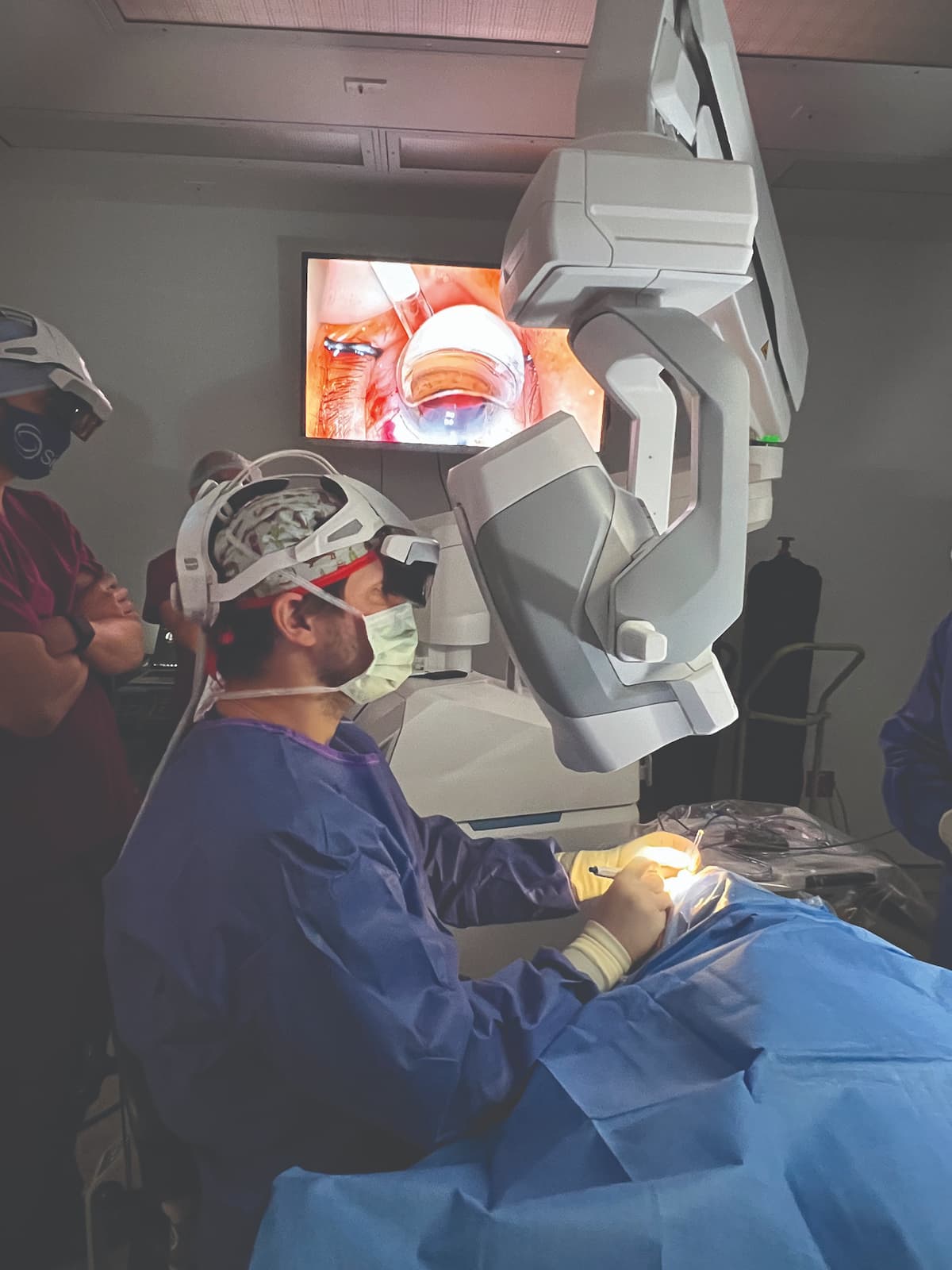
Simple head gestures are used to control functions such as focus, zoom, pan, and illumination as well as to toggle through several overlays. It is also built on an open platform that will enable future integration with electronic medical records systems. Other forms of surgical integration can also help streamline processes in the OR. Systems that bring preoperative planning data into the OR and promote intraoperative guidance, such as Callisto eye (Carl Zeiss Meditec), ORA System (Alcon), and Ally Adaptive Cataract Treatment System (Lensar). The use of such technologies can lead to a time savings of 1 to 2 minutes per patient.
Digital visualization systems are also an invaluable tool to teach and train residents and fellows. They can enjoy a simultaneous view of the surgical field and benefit from watching mentors either remotely or in the OR.
Digital visualization is an evolution, much like going from the use of loupes to a traditional microscope in the OR. If you told somebody today that they had to do cataract surgery with loupes, they would say you were crazy. I believe we are going to see the same transition occurring with digital microscopy within the next
5 to 10 years.
In addition to the benefits mentioned previously, 3D surgery is ergonomically friendly, allowing surgeons to adopt a more natural posture while operating, which increases efficiency, productivity, and professional longevity. This will be important as we continue to see more and more aging patients present for cataract surgery. I believe that 3D surgical systems are the missing link in the digital ecosystem that we are now creating within ophthalmology.
Avoid complacency
It can be easy to become complacent in the OR by using techniques and technologies that you are used to. The key to efficiency, however, is to stay abreast of new technology. Use the evolution of products to drive improvements in efficiency.
I have found that keeping an open mind and trialing new technologies has helped increase my efficiency and made me a better surgeon. I build in time to trial new devices because it takes time up front to get comfortable with any new technology. I am often surprised, however, with the amount of time savings on the back end. Complacency, on the other hand, can cost you time over the long term.
Conclusions
The time and effort you invest in maximizing efficiency metrics in your OR can be fruitful for the whole flow of your practice. It can also help build team morale and staff buy-in, which in turn can fuel the patient experience.
Start by maintaining a routine surgical technique, simplifying surgical steps, and focusing on achieving precise and effective movements. From there, consider making small changes to further streamline efficiency, including the use of preloaded IOLs and digital visualization systems. Lastly, avoid becoming complacent in your surgical technique and with the instrumentation that you use. Upgrading to advanced technologies such as phaco machines and surgical integration systems, when possible, can further boost efficiency and make your surgery days run smoother and be more rewarding.

Eric D. Rosenberg, DO, MScEng
E: ericr29@gmail.com
Rosenberg is a cornea complex anterior segment surgeon at SightMD in Babylon, New York; an assistant professor at Westchester Medical Center, New York Medical College, in Valhalla, New York; and cofounder of the Digital Ophthalmic Society. He is a consultant to Alcon, BVI Medical, and Carl Zeiss Meditec.
